SARA Issues Paper
Preventing Maternal Mortality
through Emergency Obstetric Care
April 1997
May Post, MD, DPTM
Public Health Advisor
Support for Analysis and Research in Africa (SARA) Project
The SARA Project is funded by the U.S. Agency for International
Development (AFR/SD/HRD)
The SARA Project is operated by the Academy for Educational Development with Subcontractors Tulane University, JHPIEGO, Macro International, Morehouse School of Medicine, Population Reference Bureau, and Porter Novelli. SARA is funded by the U.S. Agency for International Development (AFR/SD/HRD) under Contract number AOT-0483-C-2178-00 (Project number 698-0483).
Table of Contents
I.
Rationale for Increased Focus on Emergency Obstetric Care
II. Barriers to Timely and Appropriate EOC
2.1
Barriers to Receiving Care After Arriving at an EOC Facility
2.2
Barriers to Reaching a Facility with EOC Capabilities
2.3
Factors Influencing Decision to Seek Care Under Emergency Conditions
III. Lessons Learned and Best Practices for Improving EOC
3.1
Community Education and Involvement
a. Community
Education to Make Early Decision to Seek Care
b. Community
Involvement
- Training Community Motivators
- Formation of Community Blood Donor Associations
- Establishing Community Loan Funds
3.2
Strengthening the Referral System
a. Training
Traditional Birth Attendants
b. Emergency
Transport
c. Expanding
Midwifery Services
d. Maternity
Waiting Homes
e. Upgrading
Health Centers
3.3
Improving Quality of EOC
a. Training
in Life Saving Skills
b. Improving
Interpersonal and Counseling Skills
c. Expanding
the Roles of Non-Physician Health Care Providers
d. Ensuring
Availability of Drugs and Supplies
e. Improving
Management
V.
Research Needs and Information Gaps
VI. Conclusions
and Recommendations
Preventing Maternal Mortality
through Emergency Obstetric Care
I.
Rationale for Increased Focus on Emergency Obstetric Care
All pregnant women are at risk of obstetric complications. Most life-threatening complications occur during labor and delivery, and these cannot all be predicted. Prenatal screening does not identify all of the women who will develop complications (Rooks, Winikoff, and Bruce 1990). Women not identified as "high-risk" can and do develop obstetric complications. Most obstetric complications occur among women with no risk factors.
For example, at a health center in Kasongo, Zaire, a prenatal care program
was implemented where pregnant women were screened for their risk of developing
obstetric complications. Those coming in with a bad obstetric history (history
of stillbirths, medical intervention during delivery) were identified as
"high-risk" for developing obstructed labor. The Kasongo data showed that
only 29 percent of women who actually did develop obstructed labor were
from the "high risk" group. More than two-thirds of the women who developed
this complication were not predicted by the screening program (Kasongo
project team 1986).
Similarly, evidence that obstetric complications are common despite intensive prenatal care and screening was illustrated in a study of deliveries in non-hospital birth centers in the United States (Weatherby 1990). In that study, one of every thirteen women categorized as "low-risk" and receiving intensive prenatal care developed serious complications.
Every pregnant woman needs access to facilities with capabilities to provide emergency obstetric care (EOC)1. Neither effective prenatal care nor identifying risk will help women if EOC is not available, not accessible, or not utilized.
1 EOC includes specific interventions to manage
"emergency" obstetric complications. Interventions may be intravenous antibiotics,
oxytocics or anti-convulsants, management of abortion complications, management
of postpartum bleeding, assisted delivery for prolonged labor such as vacuum
or forceps delivery, blood transfusion, and/or cesarean section.
The Safe Motherhood Initiative was launched in 1987 -- fully a decade ago. The prime goal of the Initiative was to reduce the number of maternal deaths by half by the year 2000. Yet, new estimates of maternal mortality indicate that globally in 1990, some 585,000 women died from complications of pregnancy and labor -- 80,000 more than earlier estimates had suggested (WHO 1996).
More than 99 percent of the deaths occurred in developing countries, where maternal mortality ratios range from an average of 190 per 100,000 live births in Latin America and the Caribbean to 870 per 100,000 in Africa (WHO 1996). It also is estimated that the majority or 75 percent of maternal deaths are direct obstetric deaths due to obstetric complications such as hemorrhage, unsafe abortion, hypertensive disorders, sepsis, and obstructed labor.
To date, the focus of safe motherhood programs in most countries has been on delivery of maternal services other than emergency obstetric care. The goal of reducing maternal mortality cannot be achieved if prompt adequate care is not available for obstetric complications. The challenge now is to shift focus and concentrate on improving efficient delivery of care for emergency obstetric complications in addition to ongoing maternal health care services.
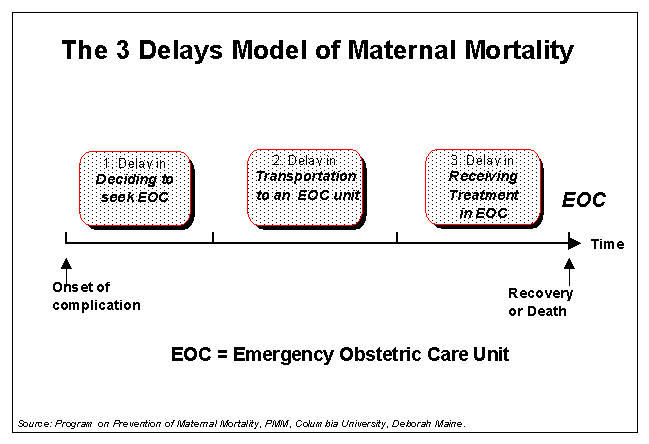
II.
Barriers to Timely and Appropriate EOC
The "3 Delays Model" developed by the Prevention of Maternal Mortality (PMM) Network identifies the points at which delay to EOC can occur:
2.1 Barriers to Receiving Care After Arriving at an EOC Facility
Studies carried out at facilities providing comprehensive EOC showed
delay in treatment once women arrive at the facilities to be a major contributing
factor to maternal mortality -- with admission-to-treatment intervals ranging
from a mean time of 2.6 hours to 15.5 hours (PMM Network 1995). Long admission-to-treatment
intervals were attributed to shortage or lack of essential supplies
and equipment, including drugs, gloves, sutures, and anesthetic
agents at the facilities, forcing the patient to wait while relatives try
to acquire required drugs and supplies in private pharmacies. In Senegal's
Kaolak hospital for example, transfusion was not available for 80 percent
of women referred in labor needing transfusion, nor was anesthesia available
for 64 percent of those who needed it (Region medicale de Kaolak 1988).
Difficulty obtaining blood for transfusion is a major
obstacle in the management of obstetric emergencies. For example, a study
in rural Tanzania concluded that the difficulty in obtaining blood was
responsible for 35 percent of maternal deaths (Price 1984). In a study
at the University of Nigeria Teaching Hospital in Enugu, the survival rate
for patients with ruptured uterus who were unable to have a blood transfusion
was 57 percent compared to a survival rate of 76 percent for patients who
received blood transfusion (Megafu 1985). Most of the health care facilities
studied either did not have blood banks or had blood banks that were inadequately
stocked (PMM Network 1992).
Lack of adequate operating theater space at the facility
also contributed to treatment delays, since obstetric emergency cases had
to compete with other surgical cases for the single general operating theater.
The delays were found to be shorter during the weekends when the operating
theater was more accessible because no general surgery cases were scheduled
(PMM 1995).
Focus group surveys with community members identified lack of drugs, blood, essential supplies, and equipment as major barriers. The strongest concerns voiced after lack of supplies, were shortage of staff and shortage of competent staff trained to manage obstetric complications (PMM 1992). For example, a study in four regions of Tanzania indicated that delayed diagnosis or inappropriate management or both were implicated in 36 percent of maternal deaths (Mtimavalye 1984).
Lack of appropriately trained staff was also a major problem identified in a community-based study of maternal mortality undertaken in Zimbabwe during a two-year period from 1989 to 1990 (Fawcus et al. 1996). Avoidable curative-care factors were responsible for 87 percent of maternal deaths in the rural study area and for 70 percent of maternal deaths in the urban study area. The study identified inadequate treatment by incompetent staff -- specifically inadequate resuscitation of women suffering from hemorrhage and septic shock, insufficient antibiotic therapy and inadequate skills in surgery and anesthesia -- as avoidable factors for maternal mortality.
Lack of supervision of staff was an additional avoidable
factor for maternal mortality identified in the Zimbabwe study (Fawcus
et al. 1996). The study reported that the responsibility for managing emergency
complications often was shouldered by relatively junior staff who failed
to diagnose/recognize the severity of the complications. This was further
compounded by limited supervision of the junior medical staff.
In a study in Tanzania, complacency attitudes among staff
was identified as one of the major barriers (Mbaruku and Bergstrom 1995).
The study found that most of the staff were convinced that maternal deaths
were due to circumstances beyond their control such as delayed arrivals,
cultural factors, and lack of drugs and equipment. All these reasons justified
passivity especially when coupled with low staff morale due to low pay.
Staff tended to forget their potential capacity to solve problems and few
or no attempts were made to look for appropriate solutions to obvious problems.
2.2Barriers to Reaching a Facility with EOC Capabilities
Once a decision has been made that a complication needs medical intervention,
availability of transportation and easy accessibility to a facility with
EOC capabilities become factors of paramount importance. The Zimbabwe maternal
mortality study reported unavailability of transportation contributed to
28 percent of deaths in the rural study area and 3 percent of those in
the urban study area (Fawcus et al. 1996). The study also reported that
among the deaths in the rural area, seven were women who had been staying
in a specially designed shelter (similar to a maternity waiting home) as
advised, but died because of the need for transport to a higher referral
level.
In most areas, no ambulances are available and in remote villages, no
car passes for days. In addition to distance and unavailability
of public transportation, other factors such as condition
of the roads (in several PMM sites, traveling on bad roads itself
was considered a cause of hemorrhage), and travel costs have
been identified as barriers to reaching a facility. Some focus group participants
indicated they would go to a traditional practitioner closer by rather
than risk the frustration and expense of going to a distant facility (PMM
1992). Distribution of facilities is another barrier. Facilities
that exist are more often concentrated around urban areas and studies have
repeatedly shown that urban dwellers have better access to health facilities
than rural inhabitants (Thaddeus and Maine 1990).
2.3
Factors Influencing Decision to Seek Care Under Emergency Conditions
Even where facilities with capabilities for EOC are easily accessible, women may not use them. In the Zimbabwe study, delay in the decision to seek care contributed to 32 percent of deaths in the rural study area and 28 percent of those in the urban study area (Fawcus et al. 1996).
Women's status in the immediate and extended family generally underlies and shapes the decision to seek care (PMM 1992). Many studies show that women cannot and do not decide on their own to seek care; the decision belongs to a spouse or senior members of the family. In a survey in six Senegalese regions, 52 percent of the respondents said the decision would be made by the husband and 44 percent said another family member would make the decision (Dia et al. 1989).
Other factors influencing decision making under emergency conditions
include perceived severity of the complication. Pregnancy
and delivery are regarded as natural processes and signs and symptoms of
complications are not always recognized as reasons for concern. For example,
focus group studies in Sokoto and Zaria, Nigeria, and Bo, Sierra Leone,
showed that prolonged labor was not considered a complication and reason
to seek care until two to five days had elapsed (PMM 1992). Failure to
recognize the severity of symptoms also was cited as a major reason for
delay in seeking care in the Zimbabwe study (Fawcus et al 1996).
Societal expectations interfere with the use of health
services in emergency conditions. Delivery at home remains one way for
women to achieve status. For example, a woman who has to go to a hospital
for delivery is thought to have failed in her essential role as a woman
and is stigmatized (PMM 1992). In Benin, women of the Bariba tribe are
expected to be stoic during labor and delivery, and the woman who manages
to deliver without calling for assistance is especially esteemed (Sargent
1985).
Culture and tradition have great influence on the decision
to seek care and, therefore, on maternal morbidity and mortality. For example,
in many African settings, women's use of health facilities may be restricted
by the necessity for privacy and/or the custom that a male relative must
accompany them while traveling. For Saudi Arabian women, the requirement
that care must be given by a woman has hindered the use of health care
services.
The necessity of traveling long distances ( often due to the inequitable distribution of facilities) and the lack of transport were deterrents in deciding to seek care, as was dissatisfaction with staff attitudes and performance.
Users' fees. Users' fees may influence utilization of non-emergency services, but findings from PMM studies indicate that users' fees have little impact on seeking care at an EOC facility in emergency conditions, once the decision to seek care has been made. In fact, at several PMM study sites where fees for services were introduced, although normal deliveries decreased markedly, the number of complicated cases seen did not change.
III.
Lessons Learned and Best Practices for Improving EOC
It is widely accepted by international experts that the route to safer
motherhood lies not through expensive technologies but through strengthening
and upgrading existing health systems to provide essential elements of
obstetric care to all those in need. As shown by the following best practices,
appropriate
life-saving EOC capabilities can be made available at each level of the
health system. For example, staff at a rural health post with basic
EOC capabilities would not be expected to perform a cesarean section, but
would be expected to make a correct diagnosis, resuscitate and stabilize
the patient, and refer her.
3.1
Community Education and Involvement
a. Community Education to Make Early Decision to Seek Care
The "Warmi" (woman) project funded by USAID/MotherCare in Inquisivi,
an isolated rural province in Bolivia, focused on community-level
activities, such as forming and enhancing community women's groups and
strengthening community education in order to foster greater responsibility
for self care and early decision to seek care (Kwast 1995). The project
identified and prioritized maternal and neonatal health problems prevalent
in the community using community women ("auto-diagnosis"), and in collaboration
with a local NGO active in the area, implemented community education programs
through simple booklets and radio programs. At the end of a three-year
period, the most striking result noted was the reduction in perinatal deaths
(PND) from 75 deaths (pre-intervention) to 31 deaths (post-intervention).
The project attributes the decline to: (1) safer birthing practices; (2)
knowing when to reach out for assistance; (3) better care of neonates and;
(4) increased knowledge and use of contraceptives. Although information
on obstetric complications was not recorded, a decline in PND indirectly
reflects a decline in some obstetric complications, such as obstructed
labor and antepartum hemorrhage (third trimester bleeding), which are important
causes of PND. Increased use of family planning in the area also may have
had an effect on maternal mortality due to abortion.
Often, traditional birth attendants (TBAs) and community members know
that a woman will die from bleeding or from eclamptic convulsions, but
they frequently wait too long to seek care at a health facility (See Factors
Influencing Decision to Seek Care Under Emergency Conditions). In the PMM
study areas in Nigeria, Ghana, and Sierra Leone, community
information campaigns using local channels of communication, such as town
criers and community meetings, have been used for community information
campaigns. The information includes danger signs during pregnancy and labor,
where to go when a complication occurs, and what the initial costs will
be.
b. Community Involvement
Training Community Motivators
In Sierra Leone and Nigeria, community motivators were
trained to improve community awareness of obstetric complications, to establish
village action groups for community loan funds, blood donation and emergency
transport, to establish links with pregnant women in the community, and
to facilitate referral for women with complications. About two-thirds of
the cost of this activity came from PMM project funds and the remaining
one-third came from the host government and the community.
Formation of Community Blood Donor Associations
Lack of blood is a constant problem that can delay treatment and result
in death. Two PMM project areas in Ghana and Nigeria established
community blood donor associations to increase voluntary blood donation.
These associations were established through community mobilization sessions
and non-cash incentives, such as certificates of honor, free blood screening,
and priority assurance if a family member needed blood.
Establishing Community Loan Funds
Lack of money to buy essential drugs and supplies for EOC has been identified as one barrier to receiving treatment for complications. In a PMM project in Sierra Leone, communities were motivated to establish community loan funds. Per capita levies were set and repayment was enforced by the community chief. Funds were managed by village development committees and loans were granted to women who could not pay for treatment. Compared to communities without community loan funds, utilization of health facilities increased for emergency obstetric care by women from communities with community loan funds during the study period. Utilization remained unchanged in communities without community loan funds.
3.2
Strengthening the Referral System
A strong referral system starts from the community level up: beginning
with trained traditional birth attendants at the community level, availability
of emergency transportation, midwives posted at the health post level,
maternity waiting homes established near a referral site, to health centers
or district hospitals upgraded to provide basic EOC or comprehensive EOC
at the first referral level.
a. Training Traditional Birth
Attendants
Following the 1978 Alma Ata conference that launched the "Health for
All by 2000" strategy, the government of The Gambia formulated
its primary health care (PHC) action plan. A key component of the PHC action
plan was the training of the traditional birth attendants (TBAs), who together
with the village health workers (VHWs), form the core of the village health
services. Under the PHC action plan, one TBA per village (from villages
with a population greater than 400) was selected to be trained. The selected
TBAs took a 10-week government training course and received birth kits
that included clean dressings, scissors, string, ergometrine tablets and
disinfectant. A study to assess the impact of the training on TBA practices
showed a significant difference in knowledge between trained and untrained
TBAs with respect to identification of high risk factors and the need for
timely referral (Post et al. 1991).
Timely referrals by trained TBAs also increased in the study area and TBAs also accompanied women with complications to the health center for delivery by a trained midwife. Maternal mortality ratio fell from 2716 per 100,000 live births to 1051, a 61 percent reduction (Greenwood 1991). However, it should be noted that the health center in the study area was upgraded to handle emergencies during the study period and emergency transport options were improved.
In some areas in Nigeria, Ghana, and Sierra Leone, the PMM teams are planning to train TBAs to provide some very basic obstetric first aid management. Hemorrhage is a major cause of maternal mortality contributing to about a quarter of direct obstetric deaths. TBAs can be taught to arrest bleeding through massage of the abdomen (fundus) or nipple stimulation, which produces uterine contractions. They also can be taught to squeeze the uterus with both hands (external bimanual compression) to slow the bleeding.
Training TBAs can have an impact on maternal health outcomes, but training TBAs alone cannot bring about significant changes in maternal mortality unless TBAs are supported by a functional referral system, effective referral facilities, and a good working relationship between the TBAs and the formal health system.
b. Emergency Transportation
Many women die while waiting for transportation or during transportation to first referral level facilities, because of the inadequacy of emergency transportation. For example in Addis Ababa, Ethiopia, 13 percent of maternal deaths recorded over a two-year period occurred on the way to the hospital. Transportation to an appropriate health facility was a major problem. In the PMM project areas, communities and associations of transport workers were mobilized to provide transport to emergency care facilities. In Sierra Leone, where vehicles are very rare at the rural level, a system was developed whereby women with complications were conveyed to a health facility in a hammock carried by four men. In Nigeria, where roads exist and cars are more common, community leaders were mobilized to collaborate with the local transport workers union to establish a roster of vehicles that could be used for emergency transportation. Union drivers were sensitized and a revolving emergency fuel fund was established. In Ghana, communities established a roster of vehicles that could be used for emergency transport in the area. In Mali, communities established community insurance funds from which money to buy up to 100 liters of gasoline for emergency transportation can be obtained. In The Gambia, the community invented motorized carts to take the women to a point where public transport and boats are available. In some parts of Africa, women's groups pool funds and lend them to various members in turn.
c. Expanding Midwifery Services
Posting Midwives at the Village Health Post Level
In Matlab, Bangladesh, government trained nurse-midwives were posted to rural health posts. The nurse-midwives were supported by a strong referral system that included a maternity clinic capable of providing basic EOC3, which in turn was supported by a district hospital with comprehensive EOC4 services. A transport system capable of referring the patient from the rural health post to the maternity clinic (via boat) and from the maternity clinic to the district hospital (via ambulance) was also in place.
3 Basic EOC includes services other than surgery
and blood transfusion. Services generally include antibiotics, sedatives
for hypertensive convulsions, oxytocics, manual removal of the placenta
for retained placenta with postpartum hemorrhage, assisted delivery such
as vacuum extraction, forceps for prolonged labor and possibly manual vacuum
aspiration for management of incomplete abortion. Basic EOC can also be
as simple as obstetric first aid to stabilize the patient before referral
(oxytocics for retained placenta, sedatives for convulsions, and antibiotics
for infection).
4 Comprehensive EOC includes basic EOC services plus
surgical and blood transfusion capabilities. Usually a district hospital
with 24-hours care.
It was reported that the mortality ratio declined substantially from
440 to 140 deaths per 100,000 births in the study area in the three-year
period 1987-1989, while in the control area the decline was not as significant
-- the mortality ratio fell from 390 to 380 (Fauveau et al. 1991). The
conclusion drawn from the study was that stationing midwives in rural areas
resulted in early diagnosis with treatment or stabilizing of obstetric
complications and increased referral to the clinic, which was staffed by
physicians (Maine et al. 1996). With a strong referral system and arrangements
for transport in place, patients from the study area were able to get to
the clinic and if necessary, from there to the district hospital in greater
numbers, and probably in better condition. In addition to posting midwives
at the village health post level, a functioning referral system was critical
to achieving the decline in maternal mortality.
Expanding Midwife Outreach Services
The referral system was strengthened in West Kiang, a rural area of The Gambia, by establishing a midwifery outreach service. Villages of 400 or more inhabitants in the area were served by a health center staffed by a government midwife, and groups of five villages were served by a community health nurse and a government-trained traditional birth attendant (TBA). Under the improved midwifery outreach service, a second midwife was posted at each village health center. This ensured increased coverage of the villages by the midwives as well as increased supervision of the community health nurse and the TBAs.
An evaluation of the project's effectiveness using a control area without
midwifery outreach service showed a greater number of referrals to the
referral hospital in the study area (both antepartum and intrapartum),
a greater number of facility-based deliveries, and a higher proportion
of women delivered by trained TBAs (Foord 1995).
d. Maternity Waiting Homes (MWHs)
Maternity waiting homes are basic structures located near a health center
or hospital for women from rural areas who are at high risk. In a rural
district of Ethiopia, setting up MWHs near a rural community hospital
for pregnant women at high risk led to a decline in maternal and perinatal
mortality (Poovan, Kifle, and Kwast 1990). The labor and the material for
building the MWHs were provided by village communities. Women using the
facility supply their own food and buy firewood locally. During the study
period, 13 maternal deaths occurred among women with complications who
were admitted directly to the hospital, compared to no mortality among
women who came to the MWH at term.
A hospital-based cohort study carried out in Zimbabwe to evaluate
the effect of stay in an MWH also found that women who stayed in MWHs had
a lower risk of poor pregnancy outcome -- namely perinatal death (PND)
-- compared to women who came directly to the hospital from home during
labor. The study found that women from the obstetric risk group that stayed
at the MWH reduced their risk of PND by nearly 50 percent compared to controls
(Chandramohan et al. 1995). The most likely mechanism for the reduced risk
of PND among women who stayed at the MWH was rapid intervention in the
event of intrapartum complications, such as obstructed labor and antepartum
hemorrhage, which are important causes of PND.
Conversely, experience in Zaire showed that the MWHs in Karawa were underutilized primarily because of a lack of community involvement in designing and building the homes and consequent lack of consideration for community concerns, particularly related to patients' food preparation.
e. Upgrading Health Centers
In Kumasi, Ghana, a general physician was trained in EOC and posted to a health center, and midwives at the health center were trained in life-saving skills. The maternity ward and operating theater were refurbished and a revolving drug fund created for procurement of essential obstetric drugs and supplies. A running water supply also was established with community involvement (Djan et al. 1996). Since upgrading the health center, the number of women with complications coming for care increased almost threefold. This indicates that where quality services are available, people will use them. Most complications were ably managed at the upgraded center and the proportion of those who had to be referred to other institutions dropped from 42 percent to 17 percent. No deaths occurred among women treated. In addition to the salary of the physician, the cost of improvements was US $30,000, mostly for equipment and supplies and came from project funds, established NGOs in the region the government, and the community.
In The Gambia, maternal mortality declined at the Royal Victoria Hospital, one of the two referral hospitals, after upgrading the health centers to basic EOC facilities. The decline was attributed to initial care received at basic EOC facilities, which stabilized the patients' conditions before referral, increasing the chances for survival. Seven health centers were upgraded and equipped to handle emergency obstetrical care and staffed with midwives and nurse-anaesthetists who had been trained in essential obstetric care, including surgical contraception. The centers were supported by two referral hospitals and, at the community level, by mobile outreach teams and government trained TBAs. Under the program, emergency transport and communications also were upgraded. A radio communication network system was established to link the health centers to the referral hospitals and ambulances were provided for some health centers.
An assessment of the Birnin Kebbi Hospital in Nigeria revealed
poor quality in care of EOC. Focus group discussions with community members
emphasized poor services as a reason for not seeking care. To improve quality,
several specialist obstetricians visited the hospital on a rotating basis
over a one-year period and provided training to general physicians on care
of emergency obstetric complications. Midwives were trained to identify
and manage obstetric complications. In addition, an obstetric first aid
box with essential drugs and supplies was introduced, and a revolving fund
was established through which drugs and supplies were made available. Since
improving quality of care at the hospital, the number of women with complications
seeking care increased while the case fatality rate dropped from 22 percent
to 5 percent (Oyesola et al. 1996).
The following case studies illustrate approaches taken to improve quality of EOC.
a. Training in Life Saving Skills
The MotherCare project, implemented in five countries including Uganda
and
Nigeria, aimed to improve the quality of maternal care by strengthening
the knowledge and skills of midwives through life-saving skills training
(Kwast 1995). The life-saving skills (LSS) training program provided midwives
with an expanded number of skills for preventing and managing obstetric
emergencies. The three-week competency-based training program includes:
In Ghana, midwives are being trained in manual vacuum aspiration
(MVA) for management of incomplete abortions and MVA has been incorporated
into Ghana's LSS training program.
b. Improving Interpersonal and Counseling Skills
Negative client-provider interactions have been identified in focus group research in several countries as a major barrier between the community and the health system. To guide client-provider interactions, the Program for Appropriate Technology in Health (PATH) in collaboration with other institutions (Georgetown University's Institute for Reproductive Health and a local NGO in Bolivia) developed a training manual to improve the interpersonal communication and counseling skills of providers. The training, focused on participatory skills, assisted providers to develop skills that enabled them to interact with clients in such a way that when information is given to the client -- such as recognition of complications, the importance of seeking care, or where to seek care -- the client can relate to the information given and therefore can make informed decisions. Most of the work related to interpersonal communication and counseling skills has been done only in Latin America and the Caribbean.
c. Expanding the Roles of Non-physician Health Care Providers
Expanding the roles of non-physicians, specifically in areas where there
are few or no doctors, play a pivotal role in preventing many needless
maternal deaths as documented by the following best practices.
In rural northwestern Zaire, selected obstetric nurses at Karawa and Wasolo hospitals were trained to perform emergency surgery, including cesarean section and surgical management of ruptured uterus (White et al. 1987). In Karawa, 278 of 321 cesarean sections were done by the trained nurse-surgeons during a period of 18 months, with two deaths (a fatality rate of 1 percent). In Wasolo, 32 cesarean sections were done by nurse-surgeons during a course of 13 months with one death. A combined total of 16 laparotomies for ruptured uterus also were performed by nurse-surgeons in Karawa and Wasolo, with only two fatalities. Without surgery, all 16 women would certainly have died.
In Ghana, the life-saving skills (LSS) training program is a continuing education project for midwives. Since 1990, nearly 400 midwives have undergone the two-week competency-based training course that provides midwives with an expanded number of skills for preventing and managing obstetric emergencies and complications. The trained midwives reported positive results including better management of postpartum hemorrhage, prolonged labor, toxemia, and infection (Taylor 1995). The results of the program indicate that with training and support midwives are capable of performing many interventions that were hitherto carried out only by physicians and obstetricians. They constitute an army of health professionals whose potential should be fully utilized.
d. Ensuring Availability of Drugs and Supplies
PMM in collaboration with hospitals, has developed "pack systems"
and "emergency boxes" of supplies for treatment of obstetric complications
in order that drugs and supplies necessary for EOC are readily available
at the facility when needed. For example, PMM teams have developed different
pack systems for treatment of leading causes of maternal mortality -- hemorrhage,
obstructed labor, sepsis, and eclampsia. Packs for cesarean section also
have been developed, which include supplies such as gauze, syringes, needles,
anesthetic agents, antibiotics, intravenous fluids, and ergometrine (Update
1994 PMM Network). Packs used in treating an obstetric complication are
then paid for or replaced by the woman's family. Other strategies implemented
to increase availability of drugs and supplies at facilities providing
services for EOC include: implementing small revolving fund schemes
to purchase essential drugs and supplies for EOC and establishing 24-hour
pharmacy services (PMM 1995). The pack system has been so well received
by some hospital management boards that similar pack systems have been
developed for treatment of illnesses other than emergency obstetric complications.
At a rural hospital in Bo, Sierra Leone, the PMM team initiated
the establishment of a cost recovery system for drugs. Essential
drugs and supplies were procured through a commercial source outside regular
government channels and emergency obstetric drug packs were then created
and made available at prices calculated to cover costs plus an 85 percent
mark-up. The drug packs were available 24 hours and prices ranged from
45 percent to 68 percent of the prices charged by the government hospital.
Of the 26 patients who received emergency drug packs during the study period,
12 paid in full and 9 paid in part, accounting for recovery of 57 percent
of charges. Those who paid in part were given credit and followed up.
e. Improving Management
The results from an intervention program at a regional hospital in Kigoma,
Tanzania,
focusing on improving hospital management to provide a conducive working
environment revealed a reduction in maternal mortality from 933 to 186
per 100,000 live births over the period 1984-1991 (Mbaruku and Bergstrom
1995). The intervention program focused on clarifying responsibilities,
delegating more responsibility to nurses and midwives, regular monthly
meetings with increased feedback, regular staff evaluation, and increased
on-the-job training programs. Other interventions included: regular maintenance
of equipment using local materials and resources, identification of norms
for patient management and referral, and development of a detailed plan
for the continuous supply of essential drugs including the initiation of
a sub-store in the maternity ward.
The improved availability of essential drugs due to the buffer effect
of the sub-store, the availability of basic working tools due to regular
maintenance schedules using local materials and resources, increased on-the-job
training programs, clarification of responsibilities, and increased feedback
and information sharing through regular meetings all resulted in significant
improvement in the skills and the morale of the staff.
The results of a hypothetical model developed to evaluate the costs of providing EOC based on a population of 300,000, 95 percent coverage, a crude birth rate of 40, hypothetical figures related to infrastructure such as the percentage of deliveries that take place in a health service location and the average occupancy rate showed the following: salaries were the largest proportion of input costs associated with provision of EOC (31 percent), followed by infrastructure improvements (16 percent), drugs (10 percent), and laboratory (9 percent). When costs were broken down by intervention, management of normal deliveries represented the largest proportion (62 percent), compared to management of obstetric complications (37 percent), and neonate management (1 percent) (Cowley 1996).
It will be important to identify the most appropriate financing and
cost-recovery measures for provision of services for EOC in different settings.
In virtually all settings, people are already paying for at least some
maternal care services. People traditionally pay traditional birth attendants
in cash or in kind for their services and buy a variety of medicines including
contraceptives. In fact, PMM studies indicate that users' fees have
little impact on seeking care at an EOC facility in emergency conditions,
once the decision to seek care has been made. Caution is needed, however,
when fees are charged to low-income women. Fee structures based on income,
fee exemptions for certain services, and subsidies for certain services
have been used successfully in some countries (Tinker et al. 1993). Subsidies
or allowances also can be provided to nurse-midwives working in remote
rural areas.
V.
Research Needs and Information Gaps
The following are research needs and information gaps that should be addressed in the development and implementation of EOC guidelines and services.
Donors, policymakers, and health planners need to recognize that the objective of the Safe Motherhood Initiative to reduce maternal mortality cannot be realized by existing services alone; that provision of EOC services in addition to existing services will be essential to bring about a sizeable decline in maternal mortality.
Providing EOC capabilities does not have to be a formidable task; it
is not an all-or-nothing proposition (i.e., either a hospital capable of
performing surgery or nothing). Based on specific settings and availability
of resources, there are interventions that can be effectively carried out
at various levels of the health system starting from the community itself
and community-level facilities such as dispensaries and health posts.
Chandramohan D, F G Cutts, and P Millard. 1995. "The effect of stay
in a maternity waiting home on perinatal mortality in rural Zimbabwe."
Journal
of Tropical Medicine and Hygiene 1995, 98:261-267.
Cowley P. 1995. "The Cost of Emergency Obstetric Care." Issues in
Essential Obstetric Care. Report of a Technical Meeting of the Interagency
Group for Safe Motherhood. May 31-June 2, 1995. New York: Family Care
International.
Dia A, et al. 1989. Maternal Mortality in Senegal: Contributing Factors in the Health System and the Community. Draft report.
Djan J O, S K Faried, S Twum, et al. 1996. "Upgrading Obstetric Care
at the Health Center Level, Kumasi, Ghana." Abstracts from the PMM Results
Conference, June 19-21, 1996, Accra, Ghana.
Fawcus S, M Mbizvo, G Lindmark, et al. 1996. "A community-based investigation
of avoidable factors for maternal mortality in Zimbabwe." Studies in
Family Planning 27(6):319-327.
Foord F. 1995. "Strengthening referral systems." Issues in Essential
Obstetric Care: Report of a Technical Meeting of the IAG for Safe Motherhood.
May 31-June 2, 1995. New York: The Population Council; Family Care International.
Greenwood A. 1991. "The Farafenni project." Presentation at the workshop
on Guidelines for Safe Motherhood Programming, November 17-21. The World
Bank/MotherCare. Washington, DC.
Kasongo Project Team. 1984. "Antenatal Screening for Fetopelvic Dystocias.
A Cost-Effectiveness Approach to the Choice of Simple Indicators for Use
by Auxiliary Personnel."
Journal of Tropical Medicine and Hygiene
87(4):173-183.
Kwast B E. 1995. "Building a community-based maternity program." International Journal of Gynecology and Obstetrics 48 Supplement 1995: S67-S82.
Maine D, M Z Akalin, J Chakraborty, et al. 1996. "Why did maternal mortality
decline in Matlab?" Studies in Family Planning 27(4):179-187.
Mbaruku G and S Bergstrom. 1995. "Reducing maternal mortality in Kigoma,
Tanzania." Health Policy and Planning. 10(1):71-78.
Mtimavalye L A, A Justesen, and E Ngawalle. 1984. Survey on Institutional
Maternal Deaths in Four Regions of Tanzania: July 1983-December 1984. Unpublished
report.
Oyesola R, D Shehu, A T Ikeh, and I Maru. 1996. "Improving Emergency
Obstetric Care at a State Referral Hospital, Kebbi State, Nigeria." Abstracts
from the PMM Results Conference, June 19-21, 1996, Accra, Ghana
Post M, A Jack, and K Manneh. 1991. Evaluation of the Traditional
Birth Attendant Training Program in The Gambia. Unpublished report
prepared for the Ministry of Health, The Gambia and the World Bank.
Poovan P, F Kifle, and B Kwast. 1990. "A maternity waiting home reduces obstetric catastrophes." World Health Forum Vol 11 1990:440-445.
Prevention of Maternal Mortality (PMM) Network. 1992. "Barriers to Treatment of Obstetric Emergencies in Rural Communities of West Africa." Studies in Family Planning. 1992. 23(5):279-291.
Prevention of Maternal Mortality (PMM) Network. 1995. "Situation Analyses
of Emergency Obstetric Care: Examples from Eleven Operations Research Projects
in West Africa." Social Science and Medicine. 40(5) 657-667.
Price T G. 1984. Preliminary Report on Maternal Deaths in the South
Highlands of Tanzania.
Journal of Obstetrics and Gynecology of East
and Central Africa. 3(103):103-110.
Rooks J, B Winikoff, and J Bruce. 1990. Technical Summary: Seminar
on "Reassessment of the Concept of Reproductive Risk in Maternity Care
and Family Planning Services." New York: The Population Council.
Sargent C. 1985. "Obstetrical choice among urban women in Benin." Social
Science and Medicine. 20(3): 287-292.
Taylor J. 1996. "Ghana Life Saving Skills Effort." Issues in Essential Obstetric Care: Report of a Technical meeting of the IAG for Safe Motherhood. May 31-June 2, 1995. New York: The Population Council; Family Care International.
Thaddeus S, and D Maine. 1990. Too Far to Walk: Maternal Mortality
in Context. New York: Columbia University, Center for Population and
Family Health.
Tinker A. 1995. Making Motherhood Safe. Washington, DC: World
Bank.
Update. 1994. Newsletter 10. Prevention of Maternal Mortality (PMM) Network.
Weatherby N. 1990. "Antepartum Assessment of Intrapartum Risk: National
Birth Center Study." Paper presented at Seminar on Reassessment of the
Concept of Reproductive Risk in Maternal Care and Family Planning Services,
New York, The Population Council.
White S, R Thorpe, and D Maine. 1987. "Emergency Obstetric Surgery Performed
by Nurses in Zaire." The Lancet 2:612-613. September 12, 1987.
World Health Organization. 1996. Revised 1990 Estimates of Maternal Mortality: A New Approach by WHO and UNICEF. WHO/FRH/MSM 96.11.


Download this article in Acrobat pdf-format Download this article in Word-format